in what view does the x-ray beam pass from one side of the body to the opposite side?
Affiliate 3
Radiographic Positioning
Linda Carlson
RADIOGRAPHIC EQUIPMENT
RADIOGRAPHIC TECHNIQUE
PATIENT Grooming
USING THE CHARTS
This chapter is designed as a quick reference guide to radiographic positioning and technique. Technical tips and supplemental views are provided to assistance in obtaining optimal movie quality using the virtually appropriate views. The routine report is highlighted in bluish; this is the minimal number of views that must be performed to accomplish a complete evaluation of the surface area in question. For further data on the views included in this chapter, a textbook dedicated to radiographic positioning should be consulted. A list of recommended further reading is included at the end of this section.
Radiographic Equipment
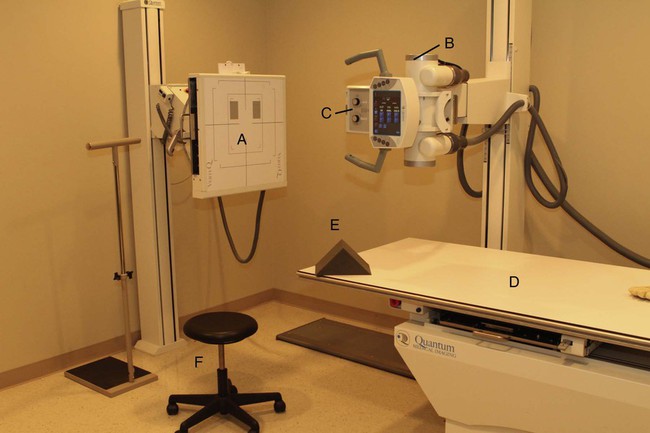
The basic components of a radiography unit are a source of radiations (x-ray tube) and a receiving medium (x-ray film in the instance of conventional patently film radiography or an energized plate in the example of computed radiography). Figures iii-1 and 3-2 identify a stool, tabular array, shields, side markers, and other accessories that are used for the radiographic setup.

Radiographic Technique
The radiographic techniques listed in this nautical chart were derived using the following parameters:
The suggested technique is within a fixed kilovolt (kV) range per torso part. In smaller patients, the lower spectrum of the kV range is used; in larger patients, the upper range of kV is used. In this organization, the milliampere-seconds (mAs) is variable, and corrections in exposure factors require changing the mAs only. To correct the exposure factors in a flick that is underexposed, the mAs must be changed by a minimum of 30% to annotation a detectable alter or by 100% for a significant change. The contrary is true for films that are overexposed. When a fixed kV system is used, merely ane exposure factor, the mAs, needs to be inverse to right for errors. The techniques contained in the nautical chart provide a starting point of adequate exposures for a radiographic system similar to the ane listed. Corrections for individual variations in machines are made by adjusting the mAs only because the chart was formulated using the stock-still kV technique.
There may be instances when a modify in penetration, or kVp, is necessary. When a film is critiqued, if the bony particular is as well light and so as to appear nonexistent, a 15% increment in kVp provides the necessary penetration. An increment in mAs is required if the bony detail is present but the overall advent of the motion picture is likewise lite.
Patient Training
Skillful patient education is essential and must include a thorough explanation of the written report beingness performed and the patient's role during the test. Protection methods and breathing instructions should be reviewed. Patients should be properly gowned, and all artifacts should be removed before the radiographic examination begins (Fig. iii-3). Female person patients in their childbearing years should exist assessed for possible pregnancy. If in that location is a possibility of pregnancy, the exam should be delayed, if possible, until information technology tin can be determined the patient is not significant, either past a negative human chorionic gonadotropin test result or the start of period. If possible, all radiographic examinations of the lumbar spine, abdomen, and pelvis should be scheduled during the first 10 days afterward the onset of menstruation because this is the least likely time for pregnancy to occur. Advisable gonadal shielding should be used in both male and female patients whenever possible.


Using the Charts
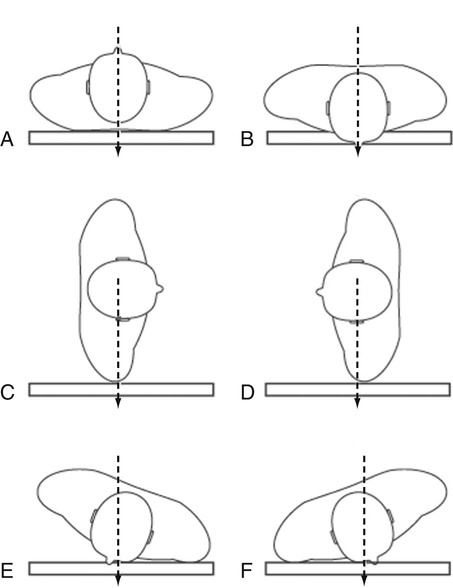
The following tables present commonly performed radiographic projections. The routine study is highlighted in blue. A routine study is the minimum number of views that must be performed to obtain a complete report of the area. Additional views are included in most sections and can exist added to the basic study. Additional views are added to better demonstrate an expanse in question or to assess movement or stability. Every bit reference, radiographic views are named past the torso part being examined and either the management the x-ray beam is passing through the torso (anteroposterior [AP]) or the portion of the trunk part touching the grid for oblique angles of the torso (correct posterior oblique [RPO]) (Fig. 3-4).
Each table explains the position setup, fundamental ray placement, tube angulation, optimal film size, and focal-pic distance for each view. To conserve x-ray moving picture and facilitate viewing, sometimes the film is divided and then that multiple views of a trunk part are seen on a single pic (Fig. 3-five). For each setup in the tables, there is a picture demonstrating the position and central ray placement and another to showroom the anatomy demonstrated past the setup. The kV and mAs section lists the type of film screen combination used and whether the study is performed with the use of a grid or tabletop. If the use of a filigree is listed, a fast film screen combination such as rare world is suggested. If detailed or nongrid is listed, a slower speed film screen combination is suggested, such as those found in extremity cassettes or 100-speed cassettes. A suggested kV and mAs range is also provided for systems described in the previous section on technique. The "Additional Information" section describes other views that may exist done to better demonstrate the desired anatomy. Technical tips are also included to aid in obtaining optimal studies.
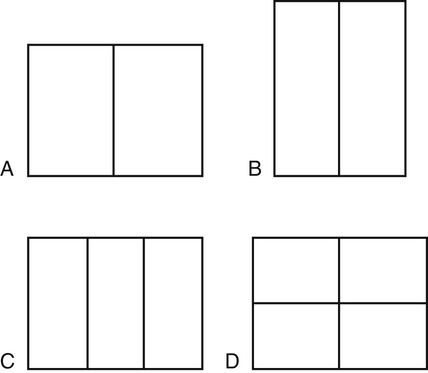
TABLE 3-1
SKULL
| Routine skull: PA Caldwell, AP Towne, Lateral Skull | |
| Position | PA Caldwell |
| Patient grooming | Remove any artifacts in the desired field (e.g., earrings, dentures, hair appliances) |
| Measurement | Place caliper base of operations at the back of the skull. Slide the caliper arm until it rests lightly at the nasion. |
| Shielding | Secure lead apron around patient. |
| Movie selection | x × 12 |
| Picture placement | Place vertical in Bucky. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Place patient with nose and forehead confronting Bucky and so the orbitomeatal line is perpendicular to the film. |
| Technique selection | kVp 70 to 80; mAs 20 to xl |
| SID | 40″ |
| Key ray placement | Using a xv-degree caudal tube tilt, key ray enters the dorsum of the skull so equally to go out the nasion. |
| Collimation | To motion picture size |
| Marker placement | Within the collimation field on either the right side or left side of patient'southward caput |
| Breathing instructions | Do not breathe. Do not movement. |
| Anatomy visualized | Frontal os, frontal and ethmoid sinuses, greater and bottom fly of the sphenoid, superior orbital fissure, foramen rotundum, orbital margins |
| Additional information | The caudal tube angle may be increased to 30 degrees to optimally define the inferior orbital rim area. Petrous pyramids announced in the lower tertiary of the orbit as performed in the preceding view. These are projected below the inferior orbital rim on the thirty-caste bending.  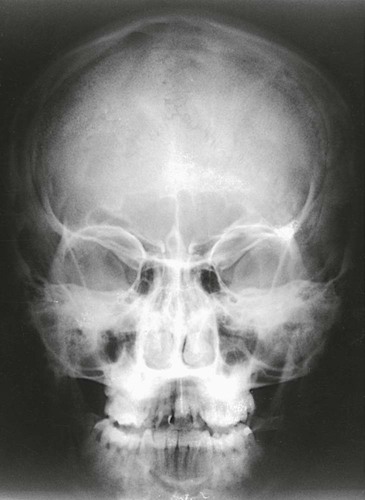 |
| Patient training | Remove any artifacts in the desired field (e.yard., earrings, dentures, hair appliances). |
| Measurement | Place base of operations bar of caliper on occiput. Slide moveable bar in toward the patient's head so as to touch the glabella. |
| Shielding | Secure lead frock around patient. |
| Film choice | 10 × 12 |
| Film placement | Place vertically in Bucky. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Place patient in AP position and so dorsum of head touches Bucky. Tuck the chin so the orbitomeatal line is perpendicular to the film. |
| Technique choice | kVp 70 to 80; mAs 30 to lx |
| SID | forty″ |
| Central ray placement | Central ray is angled 30 degrees caudally and enters 2″ in a higher place the glabella (superciliary arch). |
| Collimation | To pic size |
| Marking placement | Within the collimation field on either the right side or left side of patient's caput |
| Animate instructions | Do not breathe. Practise not move. |
| Anatomy visualized | Occipital bone, petrous pyramids, foramen magnum with dorsum sellae and posterior clinoids projected through it |
| Boosted information | If the patient cannot tuck the chin sufficiently, adjust the head tilt so the infraorbitomeatal line is perpendicular to the film and increment the tube tilt to ≈37 degrees. 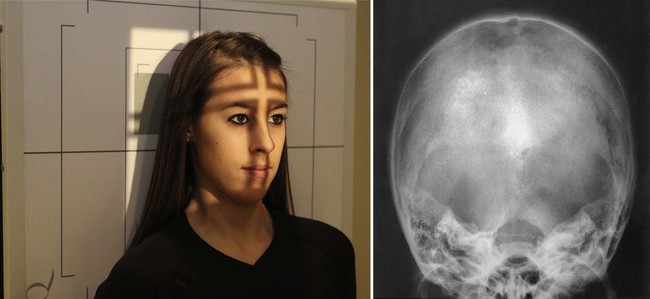 |
| Patient training | Remove any artifacts in the desired field (due east.g., earrings, dentures, hair appliances). |
| Measurement | Place the base bar of the calipers on the temporal os of one side of the caput and move the slider bar toward the patient's head so equally to touch the temporal os on the other side of the caput. |
| Shielding | Secure lead apron around patient. |
| Film selection | ten × 12 |
| Film placement | Place horizontally in Bucky. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Identify patient with side of caput confronting Bucky. Oblique the patient'south body for comfort. The interpupillary line is perpendicular to the moving picture. The external occipital protuberance and the nasion should be equidistant from the picture show to prevent rotation. |
| Technique option | kVp 70 to 80; mAs xx to 40 |
| SID | forty″ |
| Central ray placement | The central ray enters 1″ superior and anterior to the external auditory meatus. |
| Collimation | To motion picture size |
| Marker placement | Within the collimation field denoting which side of the patient'south head is touching the Bucky |
| Breathing instructions | Do not breathe. Practise non move. |
| Anatomy visualized | Lateral cranium closest to picture show, sella turcica, anterior and posterior clinoids, and ethmoid sinuses 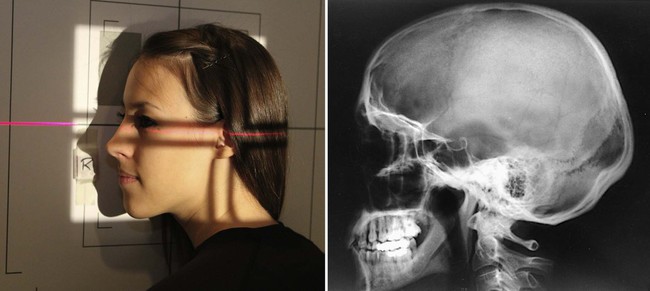 |
AP, Anteroposterior; ID, identification; PA, posteroanterior; SID, source-to-epitome distance.
Right image from Frank DF, Long BW, Smith BJ: Merrill'south atlas of radiographic positions and radiographic procedures, ed 12, St. Louis, 2012, Mosby.
Table 3-2
FACIAL BONES
| Routine Facial Bones: PA Caldwell, PA Waters, Lateral Facial Bones | |
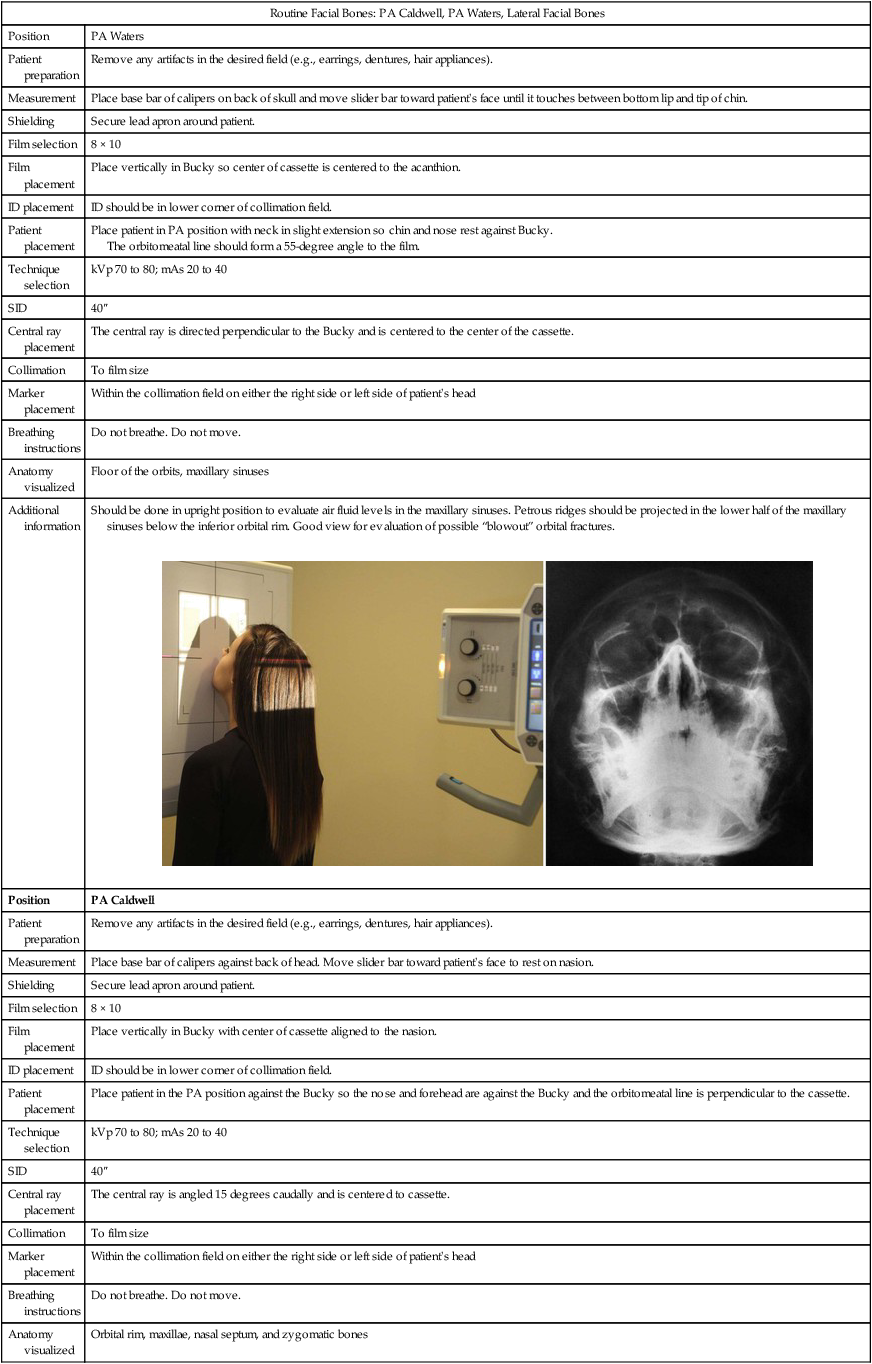
| Position | PA Waters |
| Patient preparation | Remove any artifacts in the desired field (east.thou., earrings, dentures, hair appliances). |
| Measurement | Place base of operations bar of calipers on back of skull and move slider bar toward patient's confront until it touches between bottom lip and tip of mentum. |
| Shielding | Secure lead apron around patient. |
| Film option | 8 × x |
| Picture placement | Place vertically in Bucky so center of cassette is centered to the acanthion. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Place patient in PA position with neck in slight extension so chin and olfactory organ rest confronting Bucky. The orbitomeatal line should form a 55-degree angle to the film. |
| Technique pick | kVp seventy to fourscore; mAs 20 to 40 |
| SID | 40″ |
| Central ray placement | The primal ray is directed perpendicular to the Bucky and is centered to the heart of the cassette. |
| Collimation | To moving-picture show size |
| Marker placement | Within the collimation field on either the right side or left side of patient'due south head |
| Breathing instructions | Do not breathe. Do non motility. |
| Anatomy visualized | Floor of the orbits, maxillary sinuses |
| Additional information | Should exist done in upright position to evaluate air fluid levels in the maxillary sinuses. Petrous ridges should be projected in the lower half of the maxillary sinuses below the junior orbital rim. Good view for evaluation of possible "blowout" orbital fractures. 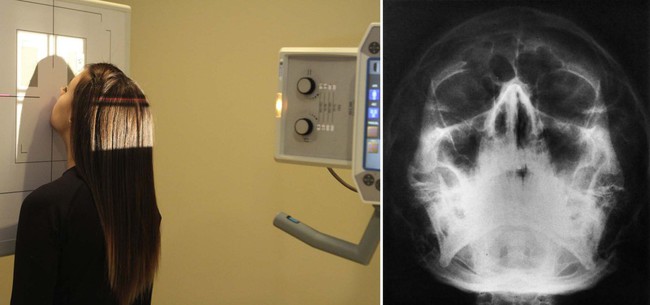 |
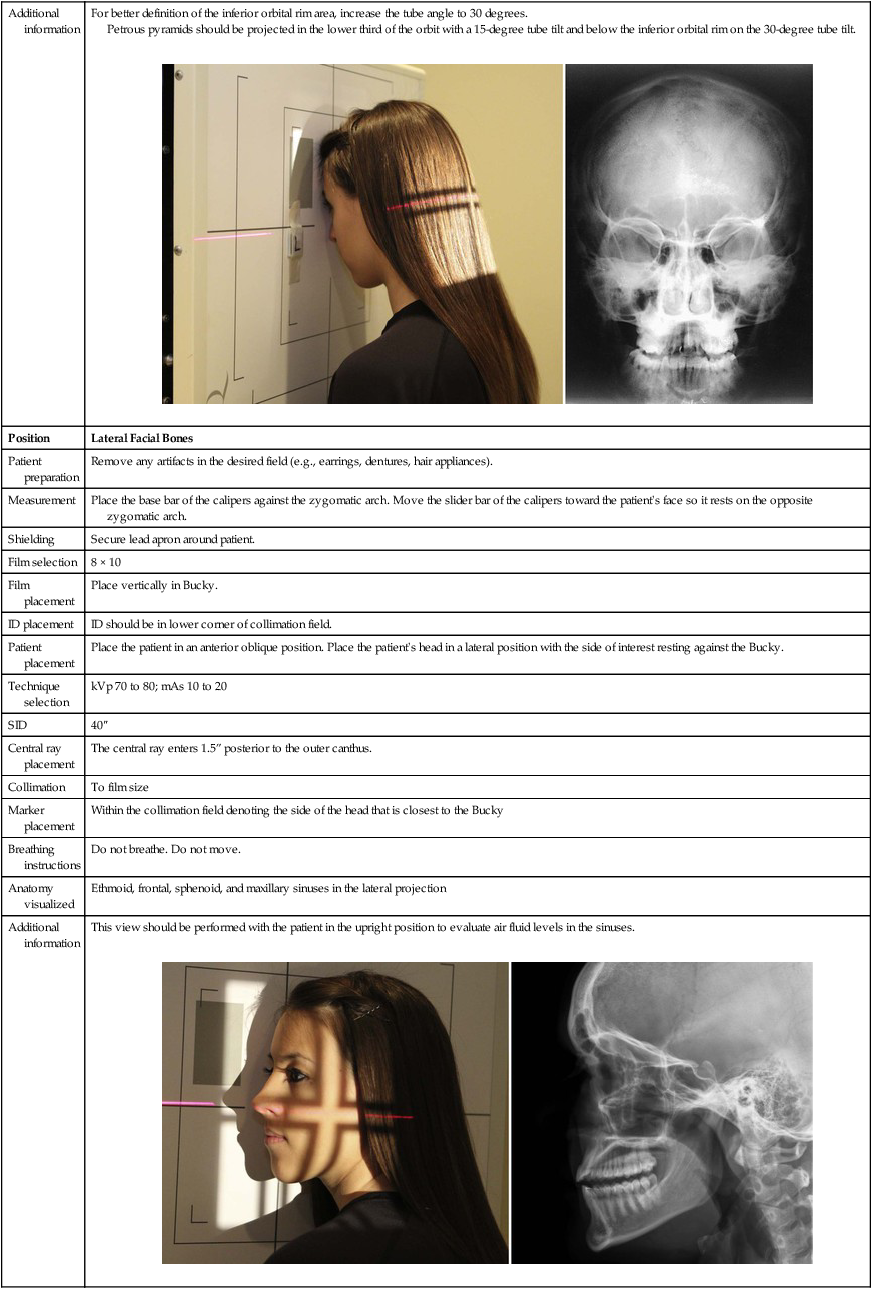
| Position | PA Caldwell |
| Patient preparation | Remove whatsoever artifacts in the desired field (e.g., earrings, dentures, pilus appliances). |
| Measurement | Place base bar of calipers against back of head. Motion slider bar toward patient'due south face to residuum on nasion. |
| Shielding | Secure lead frock effectually patient. |
| Pic selection | 8 × 10 |
| Film placement | Place vertically in Bucky with centre of cassette aligned to the nasion. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Place patient in the PA position against the Bucky and then the nose and brow are against the Bucky and the orbitomeatal line is perpendicular to the cassette. |
| Technique selection | kVp 70 to 80; mAs 20 to 40 |
| SID | 40″ |
| Central ray placement | The primal ray is angled fifteen degrees caudally and is centered to cassette. |
| Collimation | To film size |
| Marker placement | Within the collimation field on either the right side or left side of patient's head |
| Breathing instructions | Do not exhale. Do non motility. |
| Beefcake visualized | Orbital rim, maxillae, nasal septum, and zygomatic bones |
| Additional data | For better definition of the inferior orbital rim surface area, increment the tube bending to 30 degrees. Petrous pyramids should exist projected in the lower tertiary of the orbit with a fifteen-caste tube tilt and beneath the junior orbital rim on the xxx-degree tube tilt. 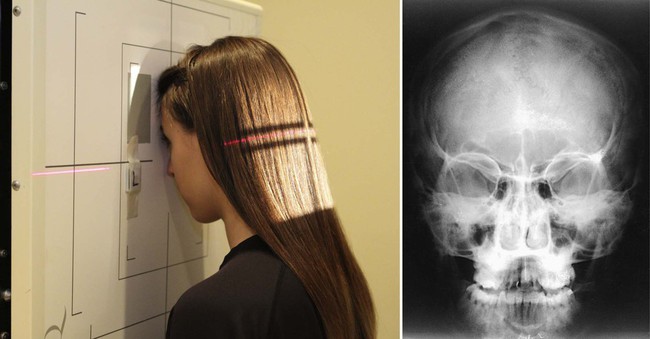 |
| Position | Lateral Facial Bones |
| Patient grooming | Remove any artifacts in the desired field (e.grand., earrings, dentures, hair appliances). |
| Measurement | Place the base of operations bar of the calipers confronting the zygomatic arch. Move the slider bar of the calipers toward the patient's face so information technology rests on the opposite zygomatic arch. |
| Shielding | Secure lead frock around patient. |
| Film pick | 8 × 10 |
| Film placement | Identify vertically in Bucky. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Place the patient in an anterior oblique position. Place the patient's head in a lateral position with the side of interest resting against the Bucky. |
| Technique selection | kVp seventy to eighty; mAs 10 to 20 |
| SID | 40″ |
| Central ray placement | The central ray enters 1.5" posterior to the outer canthus. |
| Collimation | To flick size |
| Marking placement | Within the collimation field cogent the side of the head that is closest to the Bucky |
| Breathing instructions | Exercise not breathe. Do non move. |
| Anatomy visualized | Ethmoid, frontal, sphenoid, and maxillary sinuses in the lateral projection |
| Additional information | This view should be performed with the patient in the upright position to evaluate air fluid levels in the sinuses. 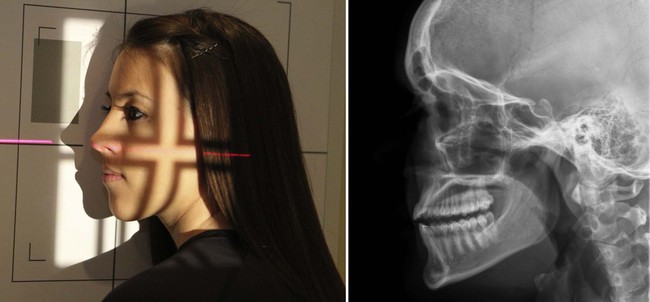 |
ID, Identification; PA, posteroanterior; RAO, right inductive oblique; SID, source-to-image altitude.
TABLE iii-3
CERVICAL SPINE: ROUTINE, TRAUMATIC, AND PALMER UPPER CERVICAL
| Routine: AP Open up Oral fissure, AP Lower Cervical, Lateral Cervical | |
| Position | AP Open Oral fissure |
| Patient grooming | Remove any artifacts in the desired field (e.g., earrings, dentures, hair appliances). |
| Measurement | Identify base bar of calipers on back of head. Instruct patient to open mouth. Move slider bar in toward patient's confront to corner of mouth (without touching patient'southward mouth). |
| Shielding | Secure pb apron around patient. |
| Film selection | 8 × 10 |
| Movie placement | Place vertically in Bucky. |
| ID placement | ID should exist in lower corner of collimation field. |
| Patient placement | Place patient in the AP position with dorsum of shoulders resting against Bucky. The plane of the upper occlusal plate and occiput with mouth open should be parallel to the flooring. |
| Technique selection | kVp seventy to 80; mAs x to 15 |
| SID | xl″ |
| Cardinal ray placement | The key ray enters the midpoint of the open up mouth. |
| Collimation | Collimate just under the optics vertically and to the mastoids horizontally. |
| Marking placement | Within the collimation field on either the correct side or left side of patient's head |
| Animate instructions | Do not exhale. Do not move. |
| Beefcake visualized | Lateral masses, anterior and posterior arches of C1, odontoid process, pedicles, lamina, and spinous procedure of C2 |
| Additional information | Correct head placement is essential. If teeth superimpose odontoid, tip head dorsum. If occiput superimposes odontoid, tip caput forward. In extreme cases, the oblique odontoid or Fuchs view may be used. 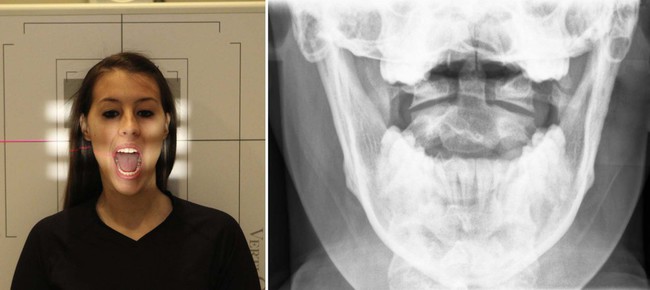 |
| Position | AP Lower Cervical |
| Patient grooming | Remove any artifacts in the desired field (e.g., earrings, dentures, hair appliances). |
| Measurement | Place the base bar of the calipers against the posterior aspect of the cervical spine at the level of C4. Motion the slider bar toward the patient until it touches the anterior attribute of the cervical spine at C4. |
| Shielding | Secure lead apron around patient. |
| Film selection | viii × x |
| Moving-picture show placement | Place vertically in Bucky. |
| ID placement | ID should exist in upper corner of collimation field. |
| Patient placement | Place patient in the AP position with dorsum of shoulders against the Bucky. The plane of the upper occlusal plate and base of operations of occiput should be parallel to the floor and so the mandible does not superimpose on C3. |
| Technique pick: | kVp 65 to 75; mAs half-dozen to 12 |
| SID | twoscore″ |
| Central ray placement | The central ray should be angled 15 degrees cephalically so as to enter the area of C4 (thyroid cartilage). |
| Collimation | To film size vertically. To mastoids horizontally. |
| Marker placement | Inside the collimation field on either the right side or left side of patient's caput |
| Breathing instructions | Exercise not exhale. Do non move. |
| Beefcake visualized | Pedicles, lamina, transverse processes, vertebral bodies, and uncinate processes of C3 to C7. Lung apices are too visualized. |
| Additional information | If mandible obscures C3 and C4, elevate mentum slightly or increase the angulation on the tube. If a lesion is suspected in visualized lung apices, a PA and lateral chest radiograph should be performed. 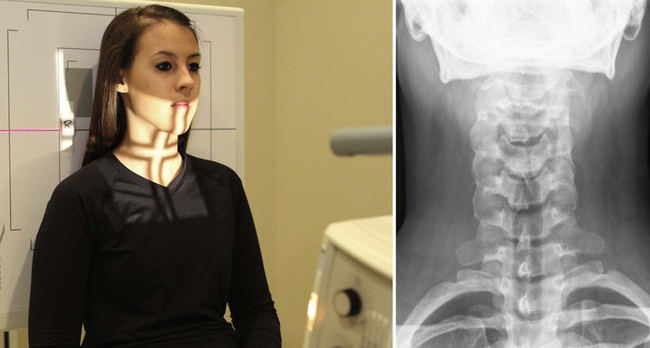 |
| Position | Lateral Cervical (Neutral Position) |
| Patient preparation | Remove whatsoever artifacts in the desired field (e.g., earrings, dentures, hair appliances). |
| Measurement | Place base bar of calipers on lateral side of patient's cervix at C4 level. Move slider bar of calipers toward patient's neck so as to rest at the C4 level. |
| Shielding | Secure lead frock around patient. |
| Film pick | viii × x |
| Motion-picture show placement | Place vertically in Bucky. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Place patient (standing or seated) next to the Bucky in the lateral position. The plane of the upper occlusal plate and the base of the occiput should be parallel to the floor. This ensures the mandible does not superimpose the inductive vertebral bodies. |
| Technique selection | kVp 70 to eighty; mAs 15 to 30 |
| SID | 72″ |
| Central ray placement: | The central ray is directed horizontally to the C4 vertebral level (approximately the level of the thyroid cartilage) and vertically through the mastoid process. |
| Collimation | To motion picture size |
| Marking placement | Within the collimation field on the side of the patient that is closest to the movie. |
| Breathing instructions | Full exhalation, to driblet shoulders |
| Anatomy visualized | Vertebral bodies, intervertebral disc spaces, articular pillars, spinous processes, and anterior and posterior arch of atlas |
| Additional Data | This the nigh important view for the evaluation of cervical spine trauma. This film should be evaluated before continuing with the remainder of the cervical series in trauma cases. If C7 is poorly visualized, a swimmer'southward view may be used. 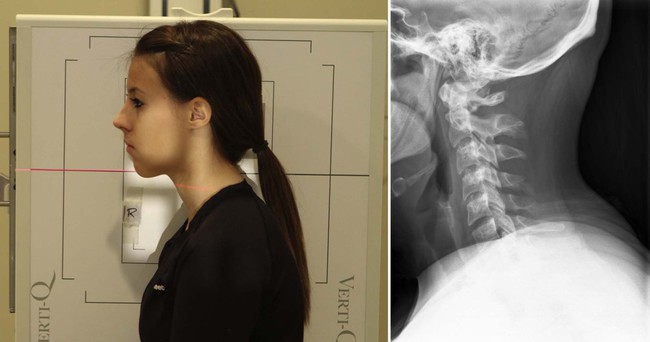 |
| Position | Lateral Cervical (Flexion and Extension: for Trauma) |
| Patient preparation | Remove any artifacts in the desired field (e.g., earrings, dentures, pilus appliances). |
| Measurement | Same as lateral cervical (neutral position) |
| Shielding | Secure atomic number 82 apron around patient. |
| Motion picture selection | 10 × 12 |
| Film placement | Identify vertically in Bucky. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Aforementioned as lateral cervical (neutral position). For flexion view, inquire patient to tuck chin into chest and roll head down so optics residuum on chest. For extension, ask patient to roll head backward, looking toward the ceiling. |
| Technique selection | kVp 70 to lxxx; mAs fifteen to 30 |
| SID | 72″ |
| Key ray placement | Same as lateral cervical (neutral position) |
| Collimation | To film size |
| Marker placement | Inside the collimation field marking the side of the cervical spine that is closest to the film |
| Breathing instructions | Full exhalation |
| Anatomy visualized | These are boosted views performed to demonstrate and evaluate excessive or macerated intersegmental mobility of the cervical spine. |
| Boosted data | Flexion and extension views should be performed but after the lateral cervical (neutral position) view has been evaluated for a gross instability. 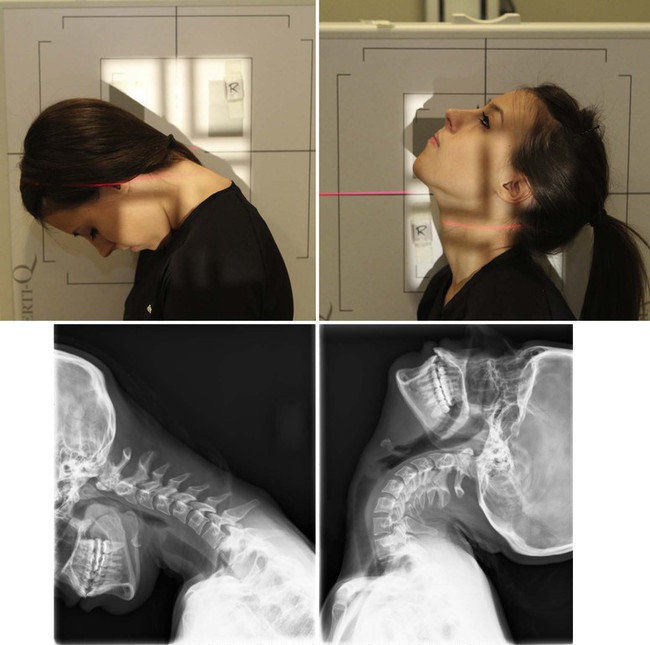 |
| Position | Cervical Oblique (for Trauma) |
| Patient preparation | Remove any artifacts in the desired field (due east.yard., earrings, dentures, hair appliances). |
| Measurement | Same as lateral cervical |
| Shielding | Secure atomic number 82 apron around patient. |
| Flick selection | 8 × x |
| Film placement | Place vertically in Bucky. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | The correct and left oblique projections may be washed in an inductive or posterior position. For anterior obliques (RAO and LAO), the anterior aspect of the patient's shoulder is placed confronting the Bucky and the torso angled 45 degrees with the grid. For posterior obliques (RPO and LPO), the posterior aspect of the patient's shoulder is placed confronting the Bucky and the body angled 45 degrees with the grid. The anterior oblique position relates less radiations dose to the thyroid gland and better accommodates the diverging ten-ray beam with the cervical lordosis. The plane of the upper occlusal plate and the base of the occiput should be parallel to the flooring to ensure the mandible does not superimpose the vertebral bodies. |
| Technique choice | kVp 70 to lxxx; mAs 15 to 30 |
| SID | 72″ |
| Central ray placement | Bending tube 15 degrees cephalically for posterior obliques or 15 degrees caudally for anterior obliques at the level of C4. |
| Collimation | To motion picture size |
| Marking placement | Inside the collimation field on the side of the patient that is closest to the Bucky |
| Breathing instructions | Total exhalation |
| Anatomy visualized | Borders of the intervertebral foramen, pedicles, facet joints, uncinates and posterior vertebral bodies. |
| Additional data | Optimal view for visualization of bony foraminal effacement resulting from cervical spine spondylosis. Optimal view for evaluation of pedicles for possible fracture and human relationship of superior and junior facet joints for possible dislocation in trauma cases. The posterior cervical oblique positions (RPO and LPO) demonstrate the contrary side intervertebral foramen (e.yard., RPO shows left foramen), and the anterior cervical oblique positions (RAO and LAO) demonstrate the same side intervertebral foramen (e.m., RAO shows correct foramen). The anterior oblique position relates less radiation dose to the thyroid, and the departure of the 10-ray beam better approximates the intervertebral disc angles; therefore, inductive obliques are typically preferred. 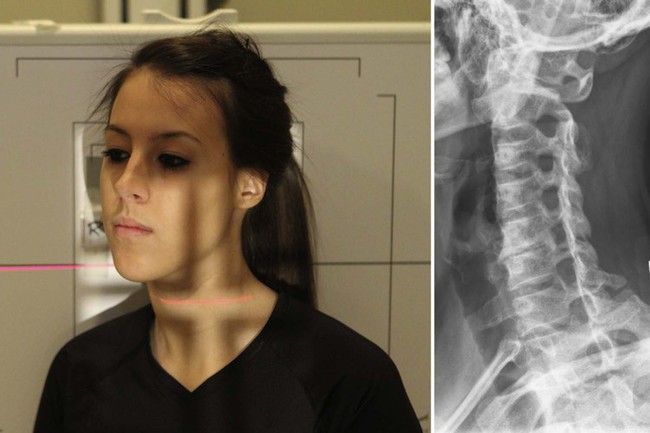 |
| Position | Oblique Odontoid (Kasabach Method) |
| Patient preparation | Remove any artifacts in the desired field (e.k., earrings, dentures, hair appliances). |
| Measurement | Utilise recommended technique. |
| Shielding | Secure lead frock effectually patient. |
| Flick selection | 8 × ten |
| Film placement | Place vertically in Bucky. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | AP with 45-degree rotation of the head |
| Technique selection | kVp 75 to 85; mAs 15 to 25 |
| SID | xl″ |
| Key ray placement | Fundamental ray is angled 15 degrees caudally to enter midway betwixt the outer canthus and the external auditory meatus |
| Collimation | To film size |
| Marker placement | Within the collimation field on the side of the head that is touching the Bucky |
| Animate instructions | Do not breathe. Do non motion. |
| Anatomy visualized | Demonstrates oblique view of odontoid process |
| Additional information | This study is performed when the odontoid cannot be visualized on an AP open mouth view. In cases of trauma or in patients with decreased range of movement, the entire body can be rotated 45 degrees. 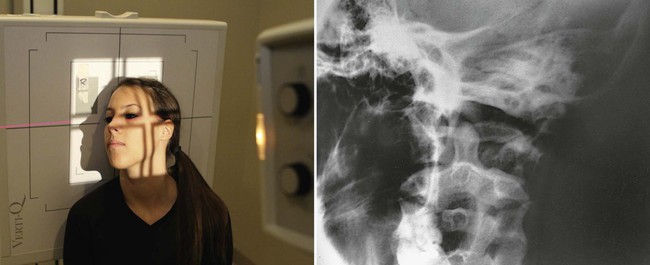 |
| Position | Fuchs (Nontrauma) |
| Patient training | Remove any artifacts in the desired field (e.g., earrings, dentures, hair appliances). |
| Measurement | Using the calipers, place the base bar under the chin. Move the slider bar and then that it touches the patient at the vertex of the skull. |
| Shielding | Secure lead apron effectually patient. |
| Film selection | eight × 10 |
| Film placement | Place vertically in Bucky. |
| ID placement | ID can be either up or down because of collimation. |
| Patient placement | Patient is in the AP position with the neck extended so the vertex of the skull touches the center of the Bucky. |
| Technique selection | kVp 70 to lxxx; mAs 10 to xv |
| SID | forty″ |
| Central ray placement | Cardinal ray is angled 0 to 15 degrees (depending on the extent to which the patient can extend his or her cervix) and enters one″ below the chin. |
| Collimation | To function size, ≈5″ × 5″ |
| Mark placement | Within the collimation field on either the correct side or left side of patient'due south head |
| Breathing instructions | Do not breathe. Do not motility. |
| Anatomy visualized | AP projection of the odontoid process as it lies within the shadow of the foramen magnum |
| Additional data | This view should not exist performed on a trauma patient or a patient with limited range of motion. Use of linear tomography may be required to better visualize the odontoid in cases of suspected fractures. This is a supplemental view used when the dens cannot be visualized on the AP open mouth view.  |
| Position | Pillar |
| Patient preparation | Remove whatever artifacts in the desired field (eastward.thou., earrings, dentures, hair appliances). |
| Measurement | Same as AP lower cervical |
| Shielding | Secure atomic number 82 frock around patient. |
| Film selection | 8 × ten |
| Film placement | Place vertically in Bucky. |
| ID placement | ID should exist in upper corner of collimation field. |
| Patient placement | Patient is in AP position with neck in full extension. |
| Technique selection | kVp 70 to 80; mAs x to 15 |
| SID | twoscore″ |
| Central ray placement | Key ray is angled 35 degrees caudally and enters midline of the cervical spine, exiting at the C7 spinous process. |
| Collimation | To film size |
| Mark placement | Within the collimation field on either the right side or left side of patient'due south head |
| Breathing instructions | Practise not exhale. Practise not movement. |
| Anatomy visualized | Shape and superlative of the colonnade |
| Boosted information | CT is the examination of choice to demonstrate pillar fractures, making this a view rarely performed. 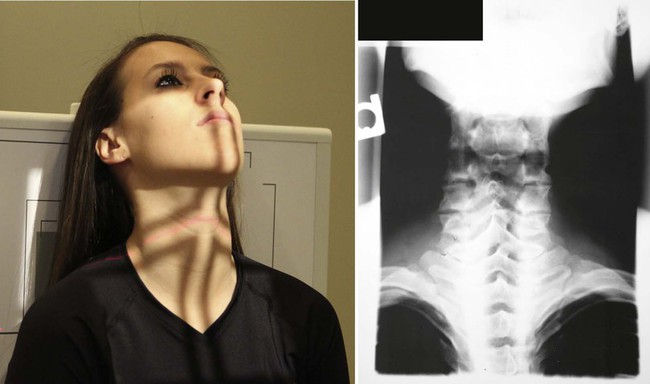 |
| Position | Vertebral Arch (AP Caudal Tilt) |
| Patient training | Remove whatsoever artifacts in the desired field (e.thou., earrings, dentures, hair appliances). |
| Measurement | Same as AP lower cervical |
| Shielding | Secure pb apron around patient. |
| Film selection | 8 × ten |
| Film placement | Place vertically in Bucky. |
| ID placement | ID should exist in upper corner of collimation field. |
| Patient placement | Patient is in AP position with neck in full extension, head obliqued. Both obliques are performed for comparing. |
| Technique pick | kVp 70 to 80; mAs ten to 15 |
| SID | 40″ |
| Key ray placement | Cardinal ray is angled 25 degrees caudally and enters midthyroid cartilage ≈3″ below the external auditory meatus, exiting at the C7 spinous procedure. |
| Collimation | To motion-picture show size |
| Marker placement | Within the collimation field denoting the side of the patient's head closest to the flick |
| Animate instructions | Do not exhale. Practice not move. |
| Anatomy visualized | Shape and continuity of the posterior curvation of the vertebrae |
| Boosted data | CT is the examination of choice to demonstrate colonnade fractures, making this a view that is rarely performed. 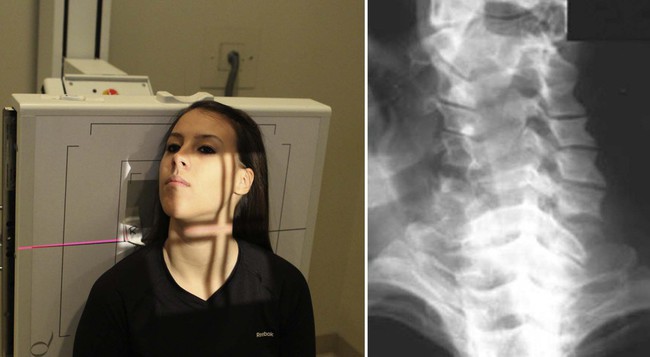 |
| Position | Nasium * |
| Patient preparation | Remove any artifacts in the desired field (e.g., earrings, dentures, pilus appliances). |
| Measurement | Using calipers, place base of operations bar at the level of the occiput. Motion the slider bar toward the patient's face until information technology rests on the glabella. |
| Shielding | Secure lead frock around patient. |
| Film selection | 8 × 10 |
| Pic placement | Place vertically in Bucky. |
| ID placement | ID should exist in lower corner of collimation field. |
| Patient placement | Patient is seated in the AP position. Bucky is tilted and then as to impact the patient's head and shoulders. |
| Technique selection | kVp 70 to lxxx; mAs 15 to 30 |
| SID | forty″ |
| Primal ray placement | Cardinal ray is angled caudally so as to enter the glabella and get out the junior tip of the mastoid process. The amount of angulation is determined by measurement obtained from the lateral cervical radiograph. |
| Collimation | To film size |
| Marking placement | Within the collimation field on either the right side or left side of patient'south head |
| Breathing instructions | Do not breathe. Practise not move. |
| Anatomy visualized | Ocular orbits, lateral masses of C1, occipital condyles |
| Additional information | Filtration is used to encompass the optics. Head clamps are used to ensure caput is held in a neutral position. This view demonstrates atlas laterality. 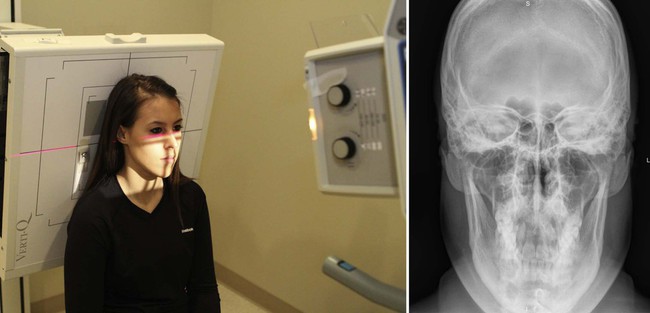 |
| Position | Base of operations Posterior * |
| Patient grooming | Remove any artifacts in the desired field (e.thou., earrings, dentures, hair appliances). |
| Measurement | Using the calipers, place the base bar at the vertex of the skull. Move the slider bar toward the patient resting the bar ane″ below the chin. |
| Shielding | Secure lead frock around patient. |
| Film choice | 8 × 10 |
| Film placement | Identify vertically in Bucky. The Bucky is tilted 45 degrees with the top of the Bucky toward the tube. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Patient is seated in the AP position with head in neutral position. The stool should be raised to its highest level. The vertex of the skull is placed in the heart of the Bucky. |
| Technique selection | kVp 75 to 85; mAs 20 to thirty |
| SID | 40″ |
| Cardinal ray placement | Central ray is angled cephalically entering 1″ beneath the mentum, passing 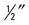 anterior to the external auditory meatus, and exiting the vertex of the skull. anterior to the external auditory meatus, and exiting the vertex of the skull. |
| Collimation | To moving-picture show size |
| Mark placement | Within the collimation field on either the right side or left side of patient'south head |
| Breathing instructions | Do not breathe. Do non move. |
| Anatomy visualized | Atlas, centrality, and nasal septum |
| Additional information | Filter out the optics. Head clamps may be used to hold head in neutral position. This view is used to demonstrate atlas rotation. The vertex may exist used as an alternate view. 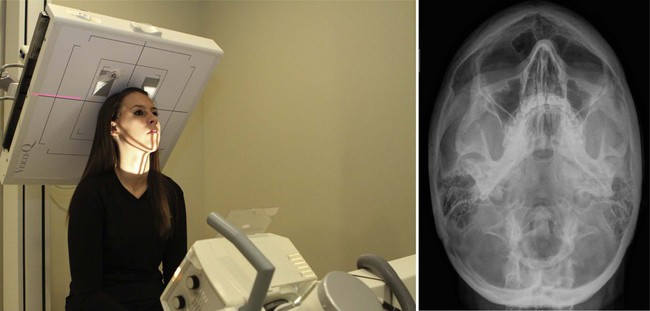 |
| Position | Palmer Open Mouth * |
| Patient preparation | Remove any artifacts in the desired field (east.g., earrings, dentures, pilus appliances). |
| Measurement | Using calipers, identify the base bar confronting the occiput. Move the slider bar toward the patient's open mouth, stopping 1 cm short of touching the face. |
| Shielding | Secure atomic number 82 apron effectually patient. |
| Moving picture selection | 8 × 10 |
| Pic placement | Identify vertically in Bucky. Bucky should exist tilted to touch the dorsum of the patient'south caput and shoulders. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Patient is seated in AP position with mouth open. |
| Technique selection | kVp 70 to 80; mAs 10 to fifteen |
| SID | 40″ |
| Central ray placement | The central ray is angled to simulate the direction of the line betwixt the upper occlusal plate and the base of the occiput (0–5 degrees) and enters at the level of the corners of the mouth. |
| Collimation | To picture show size |
| Mark placement | Inside the collimation field on either the right side or left side of patient'southward head |
| Breathing instructions | Do not exhale. Practise not move. |
| Anatomy visualized | Lateral masses, anterior and posterior arches of C1, odontoid process, pedicles, lamina and spinous process of C2, ocular orbits |
| Boosted information | Use filter to cover the ocular orbits. Head clamps may be used to hold caput in neutral position. This view demonstrates axis listing. 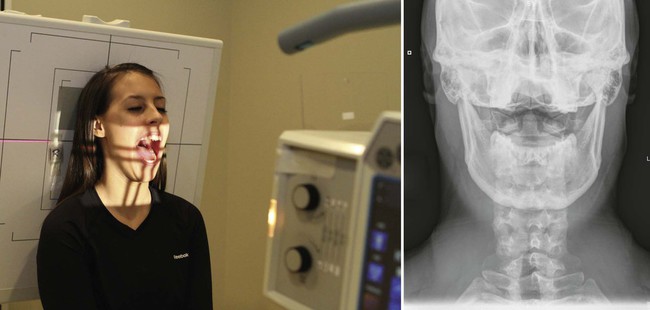 |
| Position | Palmer Lateral * |
| Patient preparation | Remove whatsoever artifacts in the desired field (e.g., earrings, dentures, pilus appliances). |
| Measurement | Using calipers, place base of operations bar against one side of patient'south neck. Move slider bar to residue comfortably on contrary side of neck. |
| Shielding | Secure lead frock around patient. |
| Film option | x × 12 |
| Motion picture placement | Place vertically in Bucky. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Patient is seated in a true lateral position with head in neutral position. |
| Technique option | kVp lxx to eighty; mAs 15 to thirty |
| SID | 72″ |
| Primal ray placement | Central ray is angled 90 degrees, perpendicular to film entering transverse process of C1 (the mastoid tip). |
| Collimation | To motion picture size vertically. Horizontally, collimate to simply behind the orbits. |
| Marker placement | Inside the collimation field on the side of the trunk closest to the motion-picture show |
| Breathing instructions | Suspend respiration on exhalation to lower shoulders. |
| Anatomy visualized | Vertebral bodies, intervertebral disc spaces, articular pillars, barbed processes, and inductive and posterior arch of the atlas |
| Additional data | This view demonstrates atlas superiority or inferiority. The measurements are as well taken off of this view to determine the tube tilt for the nasium view. 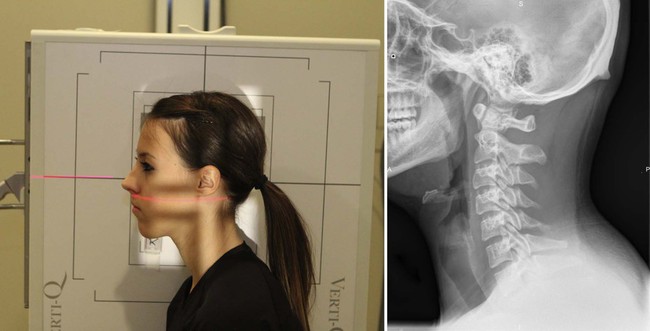 |
| Position | Vertex * |
| Patient preparation | Remove any artifacts in the desired field (e.g., earrings, dentures, hair appliances). |
| Measurement | Same equally base posterior* |
| Shielding | Secure pb frock effectually patient. |
| Film option | 8 × 10 |
| Film placement | Place vertically in Bucky. The Bucky is tilted 45 degrees then the bottom of the Bucky is closest to the tube. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Patient is seated facing the Bucky. The stool should exist lowered to its lowest level. With neck extended, the mentum should rest in the center of the Bucky. |
| Technique selection | kVp 75 to 85; mAs 20 to 30 |
| SID | forty″ |
| Central ray placement | The cardinal ray enters the vertex of the skull, passes 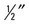 in front of the external auditory meatus, and exits 1" below the chin. in front of the external auditory meatus, and exits 1" below the chin. |
| Collimation | To film size |
| Mark placement | Inside the collimation field on either the right side or left side of patient's head |
| Breathing instructions | Do non exhale. Do not move. |
| Beefcake visualized | Atlas, axis, nasal septum |
| Boosted information | Filtration is used over the ocular orbits. Caput clamps may be used to hold the head in a neutral position. This view demonstrates atlas rotation. It is used as an alternating to the base posterior view. 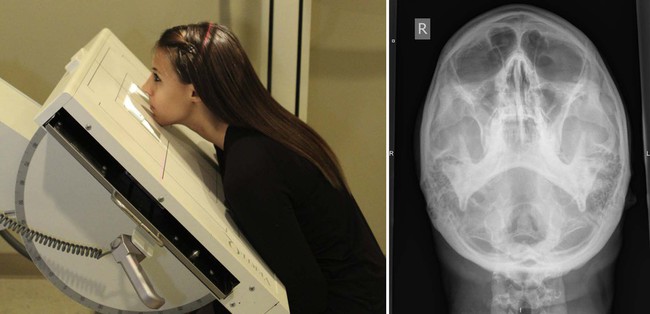 |
AP, Anteroposterior; CT, computed tomography; ID, identification; LAO, left anterior oblique; LPO, left posterior oblique; PA, posteroanterior; RAO, correct anterior oblique; RPO, right posterior oblique; SID, source-to-image distance.
*Special view used for Palmer upper cervical technique analysis.
TABLE 3-4
THORACIC SPINE, CHEST, RIBS, AND STERNUM
Simply gold members can continue reading. Log In or Register to go along
| Routine Thoracic Spine: AP and Lateral | |
| Position | AP Thoracic Spine |
| Patient grooming | Remove any artifacts in the desired field (e.g., clothing with hooks, snaps, zippers). Identify patient in gown. |
| Measurement | Using the calipers, identify the base bar on the patient's spine. Rotate the caliper so that it is over the patient's shoulder. Then motility the slider bar into the sternum of the patient. |
| Shielding | Secure atomic number 82 apron effectually patient. |
| Film option | 7 × 17 or xiv × 17 |
| Pic placement | Place vertically in Bucky. The top of the cassette should exist one″ to 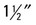 above the vertebral prominence. above the vertebral prominence. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | The patient is standing in the AP position with back against the Bucky. |
| Technique selection | kVp seventy to lxxx; mAs xx to 40 |
| SID | 40″ |
| Central ray placement | Center to the center of the cassette, ≈2″ to 4″ below the sternal notch |
| Collimation | To seven × 17 |
| Marking placement | Within the collimation field on either the right side or left side of patient'southward spine |
| Breathing instructions | Append on inspiration |
| Anatomy visualized | Vertebral bodies, intervertebral disc spaces, pedicles, spinous and transverse processes, posterior ribs, and costovertebral joints. Paraspinal lines (pleural interface) can likewise be seen. |
| Additional data | For best results, the tube should be positioned and then the anode is toward the patient's head and the cathode is down, taking reward of the "heel upshot." Wedge filtration should be used to achieve a more compatible density. The filter should be placed down to the midsternum. 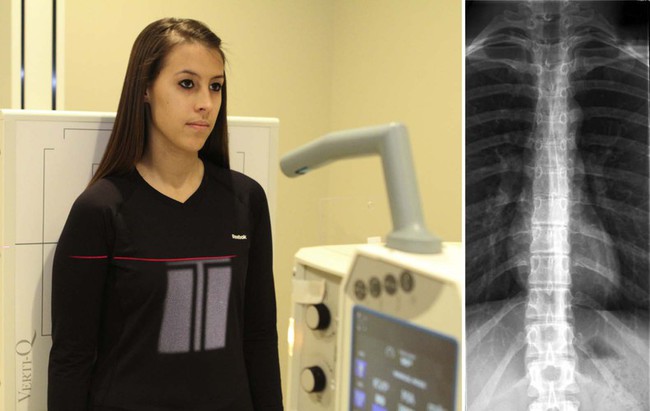 |
| Position | Lateral Thoracic Spine |
| Patient preparation | Remove any artifacts in the desired field (e.g., clothing with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Standing behind the patient, place base of operations bar of calipers under left arm. Move slider bar so as to snugly residuum under right arm. |
| Shielding | Secure lead apron around patient. |
| Film selection | 14 × 17 |
| Pic placement | Place vertically in Bucky. The tiptop of the cassette should be 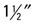 in a higher place the vertebral prominence. in a higher place the vertebral prominence. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Patient is in lateral position (depending on direction of spinal curve) with artillery raised and elbows flexed. Humeri should exist parallel to floor. |
| Technique pick | kVp 75 to 85; mAs twoscore to 60 |
| SID | 40″ |
| Central ray placement | Central ray to eye of previously placed cassette |
| Collimation | To film size vertically. To patient size horizontally. |
| Marker placement | Within the collimation field on the side of the patient that is closest to the Bucky |
| Animate instructions | Suspend on deep inspiration. Or apply the breathing technique whereby the patient takes in a deep breath and blows out slowly as if blowing through a straw (which constitutes a low mA and a long exposure time). |
| Anatomy visualized | Thoracic vertebral bodies, intervertebral disc spaces, intervertebral foramen. Upper three to four vertebrae may non be visualized because of shoulder thickness. |
| Boosted data | Utilize filtration from the lesser of the collimation field to the cross hairs of the central ray to provide a more than uniform density of the unabridged thoracic spine. If using the animate technique, use the longest exposure time with the smallest mA station that corresponds to the necessary mAs for each patient. 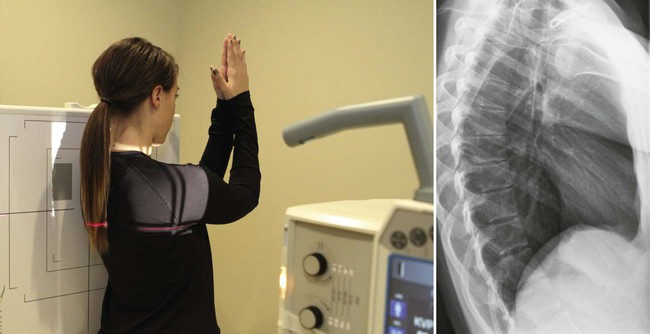 |
| Position | Swimmer'south |
| Patient preparation | Remove any artifacts in the desired field (due east.g., wear with hooks, snaps, zippers). Identify patient in gown. |
| Measurement | Same as lateral thoracic spine |
| Shielding | Secure pb frock around patient. |
| Film selection | 8 × x or ten × 12 |
| Flick placement | Place vertically in Bucky. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Patient tin can be seated or standing with arm closest to Bucky in full extension to pass alongside the ear. Shoulder nearest x-ray tube should be relaxed to its lowest bespeak. |
| Technique selection | kVp lxxx to 90; mAs fourscore to 120 |
| SID | 40″ |
| Primal ray placement | The central ray enters the T1–T2 level along the midaxillary plane. |
| Collimation | To flick size |
| Marker placement | Within the collimation field on either the correct side or left side of patient depending on which lateral is performed. |
| Animate instructions | Suspend on exhalation. |
| Anatomy visualized | Lower cervical and upper thoracic vertebral bodies and intervertebral disc spaces projected between the shoulders. |
| Boosted data | A 5-degree caudal tube tilt may aid to separate the shoulders and reduce superimposition of surrounding anatomy. This view may be used when C6-C7 cannot exist visualized on the lateral cervical view. 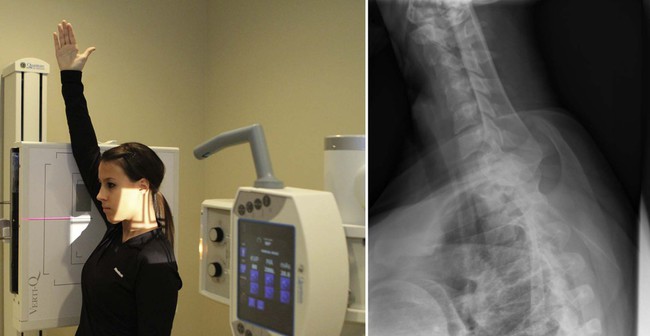 |
| Routine Breast: PA and Lateral | |
| Position | PA Chest |
| Patient training | Remove whatever artifacts in the desired field (e.k., clothing with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same every bit AP thoracic spine |
| Shielding | Secure lead apron around patient. |
| Film selection | 14 × 17 |
| Film placement | Place either vertically or horizontally in Bucky depending on width of patient. The meridian of the cassette should exist 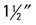 above the vertebral prominence. above the vertebral prominence. |
| ID placement | ID should exist in upper corner of collimation field. |
| Patient placement | Patient is in PA position with chest against Bucky, head straight, chin slightly elevated, and artillery rolled forrad. |
| Technique selection | kVp 110 to 120; mAs one to four |
| SID | 72″ |
| Central ray placement | The central ray is centered to the previously placed cassette. |
| Collimation | To film size |
| Marker placement | Inside the collimation field above the shoulder on either the correct or left side. |
| Breathing instructions | Deep inhalation |
| Anatomy visualized | Lungs, including apices, tracheal air shadow, heart, great vessels, and diaphragm. This view also demonstrates the costophrenic angles and bony thorax. |
| Additional information | The employ of high kVp ensures an increased grayscale on the radiograph. Poor inspiratory efforts change cardiothoracic ratio. 1 should exist able to visualize the first four thoracic vertebral bodies, seven anterior ribs, and 10 posterior ribs. In suspected upmost lesions or middle lobe infiltrates, a lordotic view may exist performed to ameliorate define these areas. If a pneumothorax is suspected, an additional view, a PA chest performed with total expiration, accentuates the visceral–parietal pleural interspace. 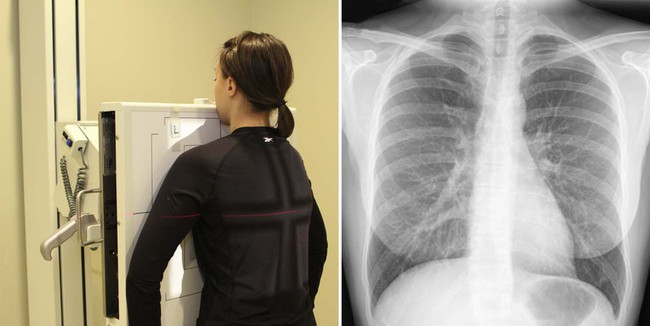 |
| Position | Lateral Chest |
| Patient training | Remove whatsoever artifacts in the desired field (e.chiliad., clothing with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same as lateral thoracic spine |
| Shielding | Secure lead apron around patient. |
| Motion picture selection | 14 × 17 |
| Movie placement | Place vertically in Bucky. Top of cassette should be 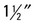 above vertebral prominence. above vertebral prominence. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Continuing with left side against Bucky with both arms in full extension raised above head. |
| Technique selection | kVp 110 to 120; mAs 4 to 16 |
| SID | 72″ |
| Fundamental ray placement | Key ray is centered to center of cassette. |
| Collimation | To flick size |
| Marker placement | Within the collimation field on the side of the patient closest to the pic merely below the ID blocker |
| Animate instructions | Deep inspiration |
| Anatomy visualized | Lungs, trachea, heart, groovy vessels, diaphragm, posterior costophrenic angles, and bony thorax |
| Additional data | The left lateral position is performed to reduce magnification of the heart shadow by having the centre closest to the film. 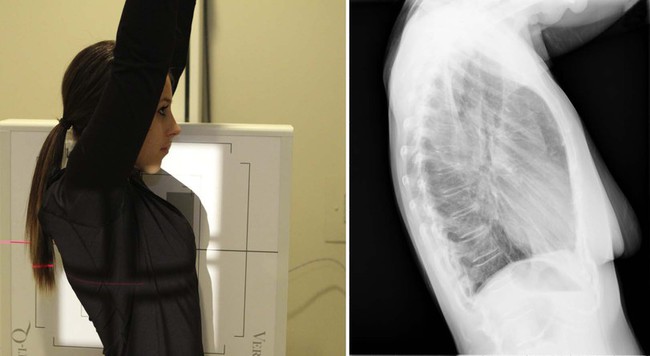 |
| Position | Apical Lordotic |
| Patient preparation | Remove any artifacts in the desired field (due east.yard., article of clothing with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same as PA breast |
| Shielding | Secure lead apron effectually patient. |
| Film option | 14 × 17 |
| Film placement | Place vertically in Bucky. Eye to fundamental ray. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | Patient is in AP position ≈1 foot from Bucky. Patient then leans dorsum so dorsum of shoulders comes in direct contact with Bucky. If the patient is unable to presume this position, she or he may stand upright, and the tube can be angled x degrees cephalic to achieve the same effect. If the patient is not able to presume this position safely, the patient may stand up upright, and a 10- to fifteen-caste cephalic tube tilt can be used. |
| Technique selection | kVp 110 to 120; mAs 1 to four |
| SID | 72″ |
| Central ray placement | Key ray enters midsternum. |
| Collimation | To film size |
| Mark placement | Inside the collimation field on either the right side or left side of patient |
| Breathing instructions | Deep inspiration |
| Anatomy visualized | This view demonstrates the apices of the lung free of superimposition of the clavicles. This view also demonstrates interlobar effusions, if present. |
| Additional information | This view may assistance to localize and ascertain any lesions suspected to be posterior to the clavicle. This view also may demonstrate infiltrate in the right center lobe. 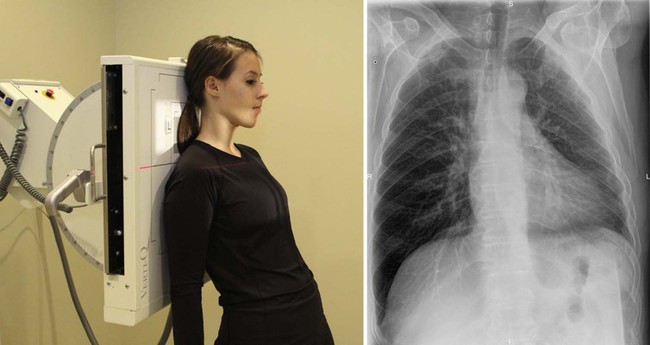 |
| Position | Lateral Decubitus |
| Patient preparation | Remove any artifacts in the desired field (e.one thousand., vesture with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same every bit PA breast |
| Shielding | Secure atomic number 82 frock around patient. |
| Film selection | 14 × 17 |
| Flick placement | Place horizontally in Bucky. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | Patient is lying on affected side (e.grand., correct side downwards for right lateral decubitus, left side down for left lateral decubitus). Arms are raised in a higher place head. Patient is placed on cart or table so the shoulders are two″ to 3″ below height of film. |
| Technique selection | kVp 110 to 120; mAs 2 to v |
| SID | 72″ |
| Central ray placement | To centre of previously centered cassette |
| Collimation | To film size |
| Mark placement | Inside the collimation field on either the right side or left side of patient |
| Breathing instructions | Deep inspiration |
| Anatomy visualized | This view is performed when the patient cannot stand and pleural effusion is suspected. Because the side down is the dependent portion of the breast, small pleural effusions may be demonstrated. This view helps delineate between pocket-size pleural effusions and scar tissue formation. |
| Boosted data | Considering pleural effusions less than 300 cc unremarkably cannot exist seen clearly on routine PA breast radiography, decubitus films should be performed if pleural effusions are suspected. 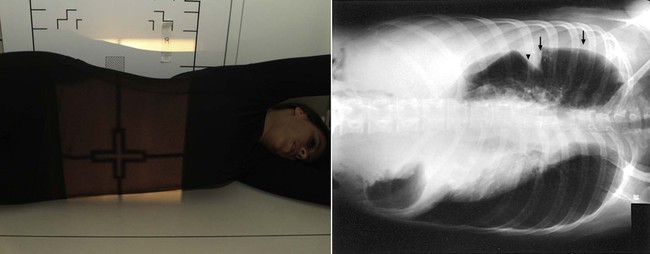 |
| Ribs: AP or PA Unilateral or Bilateral In a higher place or Below Diaphragm, Oblique, and PA Chest | |
| Position | AP Bilateral Upper Ribs |
| Patient preparation | Remove whatever artifacts in the desired field (east.yard., habiliment with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same as AP thoracic spine |
| Shielding | Secure lead apron around patient. |
| Film option | 14 × 17 |
| Film placement | Place transversely in Bucky. The peak of the cassette should exist i.5″ above the vertebral prominence. |
| ID placement | ID should be in lower corner of collimation field. |
| Patient placement | The patient is standing in the AP position. |
| Technique selection | kVp 65 to 75; mAs 20 to 40 |
| SID | 40″ |
| Central ray placement | Central ray is centered to center of cassette. |
| Collimation | To film size |
| Mark placement | Within the collimation field on either the right side or left side of patient |
| Breathing instructions | Suspend animate on full inspiration. |
| Anatomy visualized | Ribs above the diaphragm, peculiarly the posterior aspect of the ribs |
| Additional information | The nigh common surface area of rib fracture is within the axillary margin of the rib, which is not clearly seen on this projection. Oblique views are required to visualize the axillary margin of the rib. A PA chest projection should be performed to rule out pneumothorax. 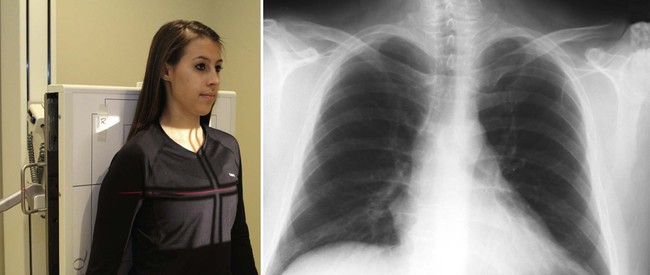 |
| Position | AP Bilateral Lower Ribs |
| Patient grooming | Remove any artifacts in the desired field (e.thou., wearable with hooks, snaps, zippers). Identify patient in gown. |
| Measurement | Measure AP through T12 area. |
| Shielding | Secure lead apron effectually patient. |
| Flick pick | 14 × 17 |
| Moving picture placement | Identify transversely in Bucky. The bottom of the cassette is i″ below the top of the iliac crest. |
| ID placement | ID should be in upper corner of collimation field. |
| Patient placement | The patient is standing in the AP position. |
| Technique selection | kVp seventy to 80; mAs 30 to threescore |
| SID | 40″ |
| Key ray placement | The central ray is directed to the center of the cassette. |
| Collimation | To film size |
| Mark placement | Within the collimation field on either the right side or left side of patient |
| Animate instructions | Suspend respiration on full exhalation. |
| Beefcake visualized | Ribs below the diaphragm |
| Additional information | A CT browse of the abdomen may be warranted to dominion out harm to the internal organs if a fracture of the lower ribs is suspected. 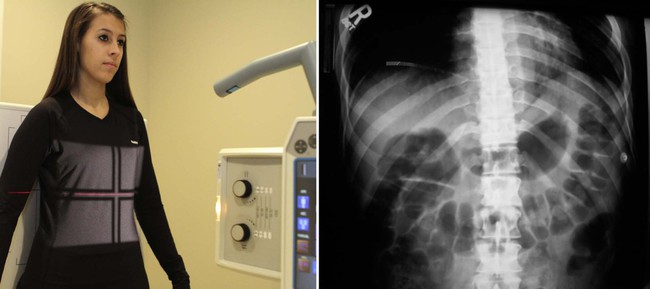 |
| Position | AP Ribs, Unilateral |
| Patient preparation | Remove whatever artifacts in the desired field (due east.grand., wear with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same as AP thoracic spine |
| Shielding | Secure lead apron effectually patient. |
| Film pick | 14 × 17 |
| Film placement | Place vertically in Bucky. The tiptop of the cassette should be ane.5″ in a higher place the vertebral prominence for ribs to a higher place the diaphragm. If the lower ribs are of interest, the cassette should be placed so the lesser of the cassette is 1″ beneath the top of the iliac crest. |
| ID placement | ID should be in the corner of the collimation field opposite the area of interest. |
| Patient placement | The patient is standing with the midclavicular plane of the affected side centered to the center of the cassette. |
| Technique option | kVp 65 to 75; mAs 20 to 40 |
| SID | 40″ |
| Central ray placement | The primal ray is directed to the center of the cassette. |
| Collimation | To film size |
| Marker placement | Within the collimation field on side of the patient that is closest to the Bucky |
| Animate instructions | For ribs above the diaphragm, suspend respiration on total inspiration. For ribs beneath the diaphragm, suspend respiration on full expiration. |
| Anatomy visualized | Ribs in a higher place or beneath the diaphragm. The view should include the area between the costovertebral joints to the axillary edge of the ribs. |
| Boosted information | This view is performed when patient presents with rib complaints on one side just. 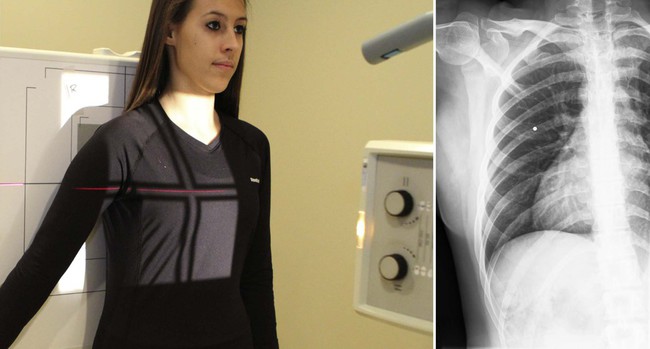 |
| Position | Oblique Ribs |
| Patient preparation | Remove any artifacts in the desired field (e.g., clothing with hooks, snaps, zippers). Place patient in gown. |
| Measurement | Same equally AP thoracic spine |
| Shielding | Secure lead apron around patient. |
| Film selection | |
Source: https://radiologykey.com/radiographic-positioning-2/
0 Response to "in what view does the x-ray beam pass from one side of the body to the opposite side?"
Post a Comment